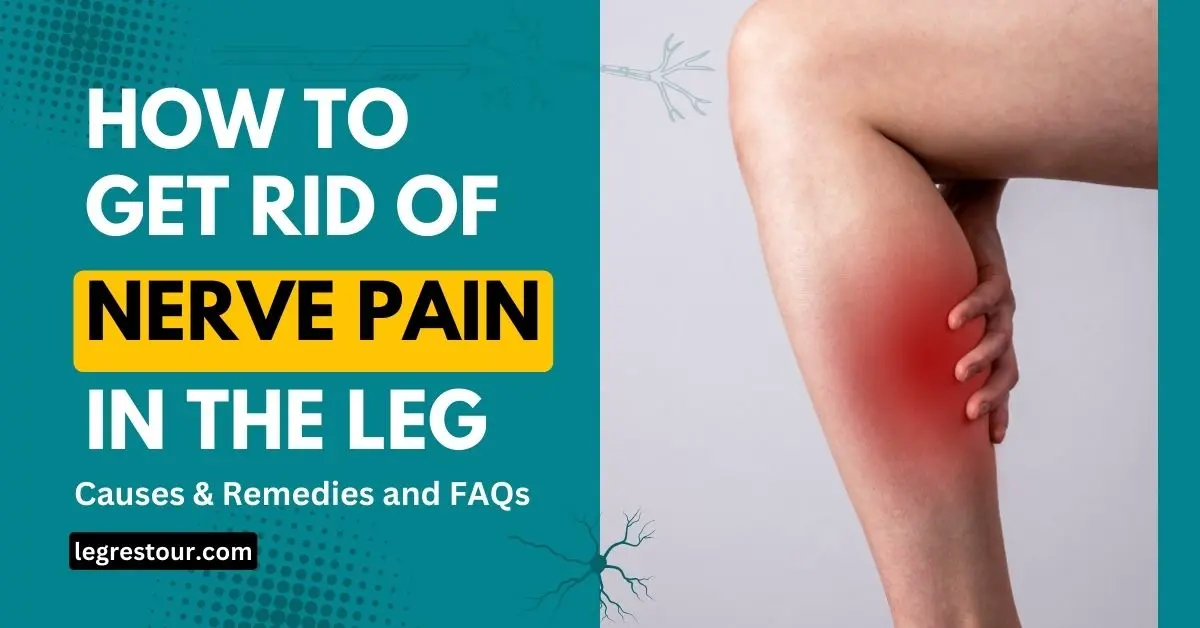
Nerve pain in the leg, also known as sciatica, can be extremely uncomfortable and disruptive to daily life. The shooting, burning, tingling or numbness that runs from the low back, through the buttocks and down the leg is often caused by compression or irritation of the sciatic nerve. The sciatic nerve is the largest and longest nerve in the body, running from the lower back down each leg. When this nerve is compressed or inflamed, it can cause debilitating symptoms. In this article, we will explore How to Get Rid of Nerve Pain in leg effective remedies and causes.
Fortunately, there are many potential remedies and treatments for sciatica leg pain that may provide relief. From home remedies to medical interventions, understanding the underlying cause and exploring various treatment options can help find an effective solution. Being informed on the common causes, self-care tips, medical treatments and frequently asked questions regarding sciatica is key to managing this condition.
Common Causes of Sciatica Leg Pain
Sciatica leg pain results when something presses against or irritates the sciatic nerve. Some common causes include:
Lumbar herniated disc
A rupture in one of the cushioning discs between the vertebrae in the lower back can allow the gel-like disc material to push into the spinal canal, compressing the sciatic nerve.
Degenerative disc disease
Discs naturally degenerate and lose hydration over time. Narrowing discs in the lumbar spine can pinch the nerves.
Spinal stenosis
When the spinal canal narrows from bone spurs or other changes, it can compress the sciatic nerve.
Piriformis syndrome
The piriformis muscle located deep in the buttocks can spasm or tighten, pinching the sciatic nerve.
Pregnancy
Weight gain, hormonal changes and baby positioning can sometimes put pressure on the sciatic nerve during pregnancy.
Injury or trauma
Impact injuries, fractures, sprains and dislocations can all potentially damage the sciatic nerve.
Tumors or growths
Very rarely, an abnormal mass growing in the pelvis or spine can press on the sciatic nerve.
Diabetes
Having high blood sugar levels associated with diabetes can cause nerve damage or inflammation.
Identifying and treating the underlying cause is key to finding lasting relief from sciatica. Consulting a doctor can help determine if any serious medical conditions are responsible for the nerve compression.
Effective Home Remedies
For mild to moderate sciatica pain caused by muscle tightness or minor disc, joint or tendon issues, home remedies may help ease symptoms. Some options to try include:
Cold packs – Applying cold packs or ice packs to the lower back and affected leg for 15-20 minutes several times per day can reduce inflammation.
Heat packs – After the first 2-3 days of cold therapy, switching to heat packs or heating pads on the area for 15-20 minutes may relax tense muscles.
Over-the-counter pain medication – Anti-inflammatories like ibuprofen, naproxen or aspirin can help relieve pain and inflammation when used for short periods. Acetaminophen is another mild analgesic option.
Physical therapy stretches and exercises – Gentle stretches and exercises tailored for sciatica can help strengthen the back and reduce nerve compression. Yoga poses or using a foam roller may also improve flexibility.
Massage – Seeing a massage therapist trained in pregnancy massage, neuromuscular therapy or other sciatica-focused techniques can loosen tight muscles pinching the nerve.
Rest – Taking frequent breaks to rest in comfortable positions, such as lying on the back with a pillow under the knees, can allow symptoms to subside.
Comfortable shoes – Wearing shoes with ample cushioning and arch support may reduce aggravation from standing or walking.
Sitting adjustments – Chairs with good lower back support, or cushions to raise and support the hips while sitting, can minimize pressure on the sciatic nerve.
While these self-care remedies may temporarily reduce sciatic nerve pain, the effects are usually short-term. More advanced medical treatments may be needed for lasting relief.
Medical Interventions
If self-care strategies aren’t providing lasting relief after a couple weeks, it’s a good idea to see a doctor. A physician can determine if the sciatica is caused by an underlying condition requiring more intensive treatment. Medical interventions might include:
Medications – Prescription medications like muscle relaxers, steroids or tricyclic antidepressants are sometimes used to calm muscles, reduce inflammation or change pain signaling.
Spinal injections – Cortisone steroid injections into the epidural space around the spinal cord may temporarily decrease inflammation pressing on the nerve.
Chiropractic adjustments – Gentle manipulation techniques can help re-align the spine to take pressure off the compressed nerve.
Acupuncture – Fine needles placed in specific points along the affected nerve pathway can block pain signals.
Surgery – For severe sciatica caused by a herniated disc or bone spur that’s unresponsive to other treatments, surgery may be an option. Common procedures include discectomy or laminectomy.
Transcutaneous electrical nerve stimulation (TENS) – A TENS unit directs mild electrical pulses to the nerve via electrodes placed on the skin, which may interfere with pain signal transmission.
Consulting with a doctor can help decide if any of these medical treatments are appropriate options based on the individual’s symptoms and underlying cause. In some cases, a combination of therapies may be prescribed. Patience is needed, as it may take some trial and error to find the most effective treatment approach.
It’s important for you: How to Relieve Foot Pain from Running
Frequently Asked Questions
1. How long does sciatica pain usually last?
For most people, acute flare ups of sciatica pain resolve within 4 to 6 weeks with conservative treatment. About 40% of individuals will still have some symptoms after 6 weeks. Chronic sciatica lasting over 3 months is less common.
2. When should you see a doctor for sciatica?
See a physician if self-care hasn’t improved pain after two weeks. Also get prompt medical attention for sciatica accompanied by progressive leg weakness, loss of bowel or bladder control, fever, or numbness in the groin or rectum area. These may indicate a serious underlying condition requiring emergency treatment.
3. Is surgery always necessary for a herniated disc causing sciatica?
No, many herniated discs heal through rest and conservative treatments. Surgery is usually only considered if the herniation is severe, or if debilitating symptoms last more than 4-6 months despite other therapies.
4. Can physical therapy help sciatica?
Yes, physical therapy including exercises to strengthen the back and stretch the piriformis muscle can be very beneficial. A physical therapist may also use techniques like massage, heat/cold therapy and TENS to provide pain relief.
5. What exercises are good for sciatica pain?
Try gentle stretches like knee-to-chest, calf stretches, child’s pose and lunges. Strengthening exercises like bridges, abdominal crunches or wall squats can also help take pressure off the sciatic nerve over time. Yoga and swimming are other good low-impact exercise options.
6. What sleeping positions are best with sciatica?
Sleeping on the side with a pillow between the knees, or on the back with a pillow under the knees, helps maintain the natural curve of the spine and minimize nerve compression. Avoid sleeping on the affected side.
7. Can sciatica cause permanent damage?
In most cases, sciatica responds well to conservative treatment and does not result in permanent nerve damage. But chronic compression of the nerve can potentially lead to weakness or numbness in the affected leg. Seeking prompt medical attention is advised.
8. Are there any risks or complications with epidural steroid injections?
Epidural steroid injections are generally very safe, but possible (rare) risks include allergic reaction, injection into a blood vessel, bleeding or infection at the injection site, headache and nerve damage.
9. How often can you get epidural injections for sciatica?
Epidural steroid injections can typically be repeated up to 3 times per year, if they provide pain relief. However, benefits tend to diminish with each injection, and they are not meant to be long-term treatment solution.
10. Can sciatica affect or cause weakness in the leg, foot or ankle?
Sciatica can potentially cause referred pain, tingling or numbness from the low back down through the leg, ankle or foot. In some cases, compression of the nerve can result in temporary muscle weakness in parts of the affected leg.
Conclusion
Living with sciatic nerve pain in the leg can be extremely frustrating. But understanding the common causes and exploring proven self-care tips, medical treatments and exercise modifications can help find relief. While symptoms may come and go, one or a combination of these options typically allows most people to effectively manage sciatica flare ups within a few months. Being proactive with conservative treatments and talking to a doctor can get you on the path to feeling better.